How to Get the GLP-1 Benefits Using Your Own Metabolism
Harnessing Diet, Time-Restricted Feeding, and Chronotherapy to Naturally Elevate Your Body's Own GLP-1
GLP-1 medications are transforming medicine, but your body already makes this powerful hormone. Learn how smart nutrition, meal timing, and lifestyle strategies can naturally boost your own GLP-1 levels for better metabolic health.

By now you have probably heard the buzz around GLP-1 medications — drugs like semaglutide and tirzepatide are transforming how we approach obesity and type 2 diabetes, and for good reason. But here is something that often gets lost in all the excitement: your body already produces GLP-1 naturally, every single day. The real question is not whether you have this hormone — it is whether your lifestyle is helping your body make enough of it, at the right time, and in the right way.
As a physician interested in functional medicine and metabolic health, I find this conversation absolutely fascinating. The pharmaceutical industry is racing to develop ever more sophisticated multi-hormonal agents that mimic and amplify what nature designed, while many of us are unknowingly suppressing our own natural production through poor meal timing, low-fiber diets, and disrupted sleep. Let us change that.
What Is GLP-1 and Why Does It Matter?
Glucagon-like peptide-1 (GLP-1) is a hormone secreted primarily by specialized cells in the lining of your small intestine and colon — called L-cells — in response to food. When you eat, these cells release GLP-1 into your bloodstream, and it does several remarkable things: it signals your pancreas to release insulin in a glucose-dependent manner, it slows the rate at which your stomach empties, it reduces appetite by acting on your brain's hypothalamus and brainstem, and it has anti-inflammatory effects throughout the body.
In short, GLP-1 is a master metabolic coordinator. It helps you feel full, keeps blood sugar stable, and protects your cardiovascular system. As outlined in leading research on incretin hormones, GLP-1 works in concert with other gut hormones like GIP, PYY, and amylin to create what we might call an integrated post-meal metabolic response — a beautifully orchestrated hormonal symphony that evolved over millions of years.
The problem? Our modern lifestyles — irregular eating schedules, ultra-processed foods, disrupted sleep, sedentary habits — are essentially tone-deaf to this symphony.
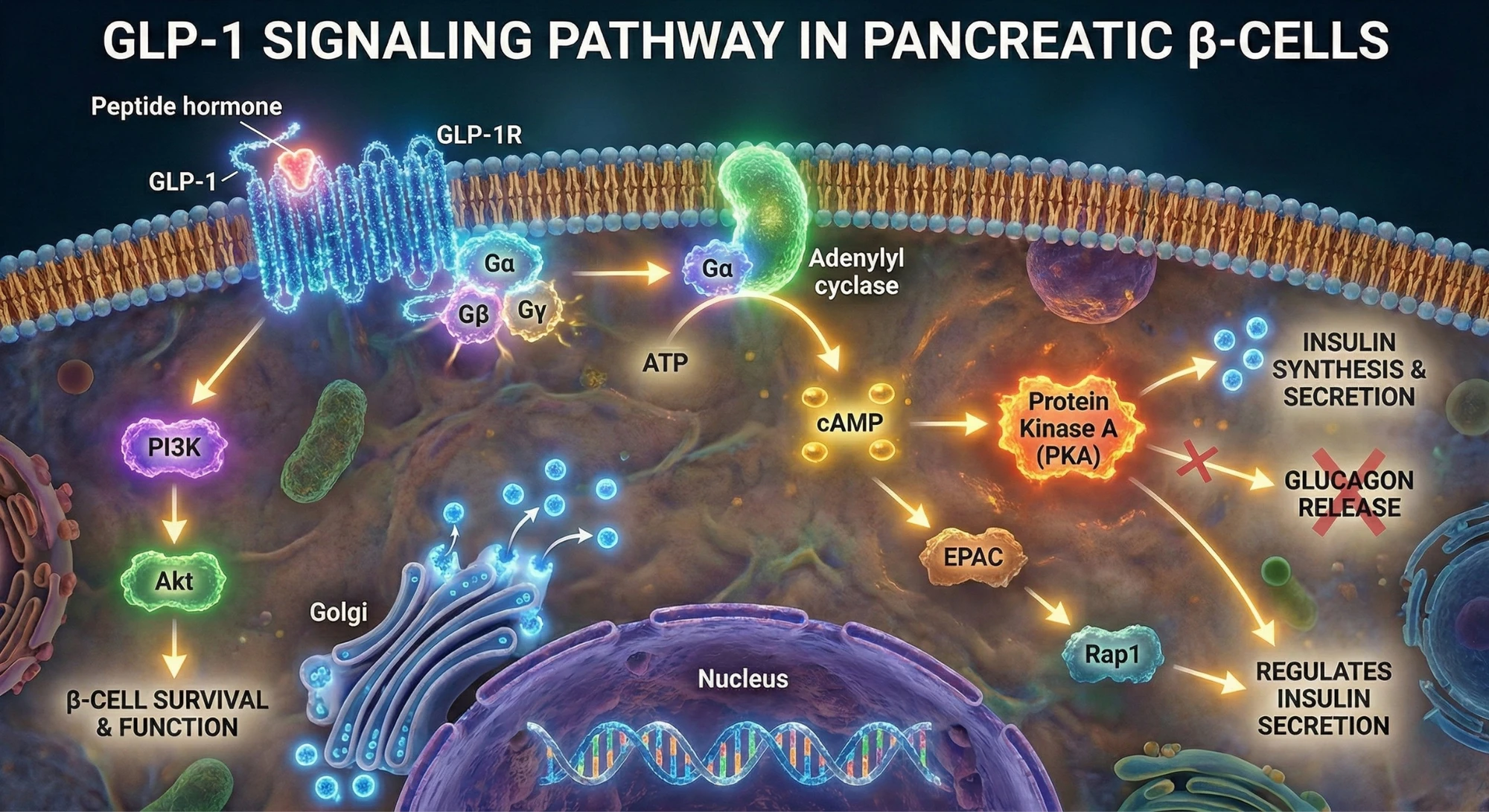
Inside your gut, specialized cells called L-cells act as metabolic sensors. They detect the nutrients passing through your intestines — particularly dietary fiber, protein, and certain fats — and respond by releasing GLP-1 directly into your bloodstream. Think of them as tiny biological pharmacies, dispensing your body's own appetite-regulating, blood-sugar-stabilizing medicine with every well-chosen meal. Understanding how to activate these cells through diet and lifestyle is the foundation of natural GLP-1 optimization.
The Metabolic Metronome: Your Body's Internal Rhythm
One of the most underappreciated concepts in metabolic health is the idea of the metabolic metronome — the idea that your metabolism is not a static engine running at a constant speed, but a rhythmic, time-sensitive system that is exquisitely sensitive to when things happen, not just what happens.
Every cell in your body contains a molecular clock — a set of genes that oscillate on a roughly 24-hour cycle, known as the circadian rhythm. Your metabolic hormones, including GLP-1, follow these rhythms. Research published in the Proceedings of the National Academy of Sciences showed that the timing of feeding itself drives gene expression rhythms in the liver and gut, independent of the master brain clock. In other words, when you eat sends a powerful signal to your metabolic machinery.
When your eating pattern is aligned with your circadian biology — front-loaded during daylight hours, with a meaningful overnight fast — your gut hormone responses, including GLP-1, are more robust. When you eat late at night, skip breakfast, or graze continuously throughout the day, you are disrupting this metabolic metronome, and your GLP-1 response suffers along with it.
Chronotherapy: Eating With the Clock
Chronotherapy — the practice of timing your health behaviors to align with your body's biological clock — is one of the most powerful and underused tools in metabolic medicine. And its impact on GLP-1 is real.
A landmark study by Sutton and colleagues published in Cell Metabolism demonstrated that early time-restricted feeding — eating earlier in the day within a narrower window — improved insulin sensitivity, blood pressure, and oxidative stress markers in men with prediabetes, even without weight loss. These benefits are partly mediated by improved gut hormone responses, including better GLP-1 pulsatility.
Similarly, research by Jakubowicz and colleagues showed that consuming a larger, nutrient-dense breakfast produced significantly greater GLP-1 responses compared to eating the same calories at dinner. Your gut's L-cells are simply more responsive earlier in the day, when your circadian biology is primed for metabolic activity.
Practical chronotherapy principles to support GLP-1: - Eat your largest, most nutrient-dense meal earlier in the day - Aim to finish eating at least 2–3 hours before bedtime - Keep a consistent meal schedule — your gut clock loves predictability - Protect your overnight fast — even 12 hours of fasting has measurable metabolic benefits

Starting your day with a substantial, whole-food meal is not just good nutrition advice — it is chronobiology in action. Your gut's GLP-1-producing L-cells are more responsive to nutrients earlier in the day, when your circadian system is primed for metabolic activity. A morning meal rich in protein, fiber, and healthy fats can trigger a significantly stronger GLP-1 response than the identical meal eaten late in the evening. The clock matters as much as the food on your plate.
Time-Restricted Feeding: Creating Space for Your Metabolism to Breathe
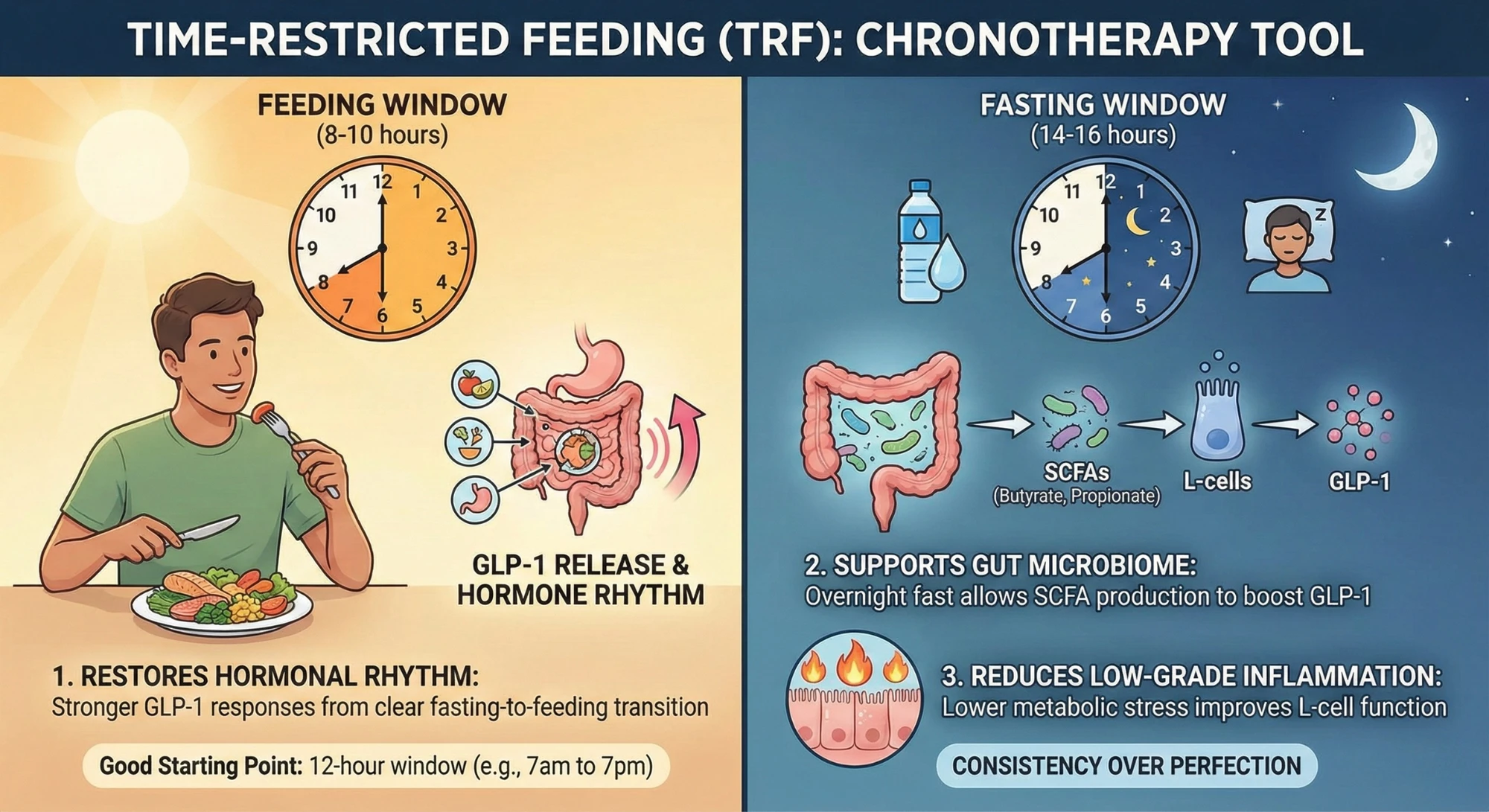
Time-restricted feeding (TRF) is perhaps the most accessible chronotherapy tool available to everyone. It simply means confining your eating to a defined window — typically 8 to 10 hours — and allowing your body a meaningful fast for the remaining 14 to 16 hours.
This approach does several things that support natural GLP-1 activity:
1. It restores the hormonal rhythm. Constant grazing blunts the pulsatile release of gut hormones. A clear fasting-to-feeding transition creates the hormonal contrast that makes GLP-1 responses more pronounced and effective.
2. It supports gut microbiome health. The overnight fast gives your gut bacteria time to ferment fiber into short-chain fatty acids (SCFAs) like butyrate and propionate — and these SCFAs are powerful stimulators of GLP-1 release from L-cells. Research by Chambers and colleagues demonstrated that targeted delivery of propionate to the colon significantly increased GLP-1 and PYY levels while reducing appetite and calorie intake.
3. It reduces low-grade inflammation. Chronic low-grade inflammation — driven by poor diet and disrupted sleep — impairs the function of gut L-cells. TRF, by reducing metabolic stress, helps restore a healthier gut environment where GLP-1 production can thrive.
A good starting point for most people is a 12-hour eating window (e.g., 7am to 7pm), gradually moving toward a 10-hour or 8-hour window as it becomes comfortable. The key is consistency over perfection.
What You Eat: Nutrition as a GLP-1 Signal
Beyond when you eat, what you eat profoundly influences how much GLP-1 your gut produces. Your L-cells are essentially nutrient sensors — and they respond very differently to whole foods versus ultra-processed ones.
Dietary Fiber and Fermentable Carbohydrates
This is arguably the single most powerful nutritional lever for GLP-1. When you eat fiber — especially fermentable, prebiotic fiber from foods like oats, legumes, vegetables, chicory, onions, garlic, and leeks — your gut bacteria ferment it into SCFAs. These SCFAs, particularly propionate and butyrate, directly stimulate L-cells to produce GLP-1 and PYY.
Research published in Science by Zhao and colleagues showed that a diet selectively enriched in diverse dietary fibers significantly increased the abundance of beneficial gut bacteria and improved metabolic markers in people with type 2 diabetes — with gut hormone improvement as part of the mechanism. Aim for at least 25–35 grams of fiber per day, from varied whole food sources.
Protein at Each Meal
Protein is one of the most potent direct stimulators of GLP-1 secretion. Amino acids — particularly from whey, eggs, legumes, and fish — trigger L-cell release of GLP-1 within minutes of entering the small intestine. Studies have shown that a higher-protein meal produces a more sustained GLP-1 and satiety response compared to a high-carbohydrate meal of equivalent calories.
This is one reason why a breakfast of eggs and vegetables tends to keep you satisfied far longer than a bowl of cereal — it is literally a more effective GLP-1 stimulus.
Healthy Fats: Olive Oil, Omega-3s, and More
Certain fats, particularly monounsaturated fats (olive oil, avocado) and omega-3 fatty acids (fatty fish, walnuts, flaxseed), also stimulate GLP-1 release and support the gut environment that produces it. Extra virgin olive oil, a cornerstone of the Mediterranean diet, has been associated with favorable gut microbiome changes and improved incretin responses.
In contrast, heavily processed seed oils, trans fats, and refined carbohydrates appear to blunt GLP-1 responses and promote gut dysbiosis — exactly the opposite of what you want.
Fermented Foods
Kefir, yogurt, kimchi, sauerkraut, and miso introduce beneficial bacteria into your gut that support a diverse, fiber-fermenting microbiome. A healthier, more diverse gut microbiome is associated with better GLP-1 production and more effective metabolic signaling overall.
Movement: The Often-Forgotten GLP-1 Booster
Physical activity is a powerful, underappreciated modulator of GLP-1. Acute exercise — even a brisk 15–20 minute walk after a meal — has been shown to enhance postprandial GLP-1 responses and improve insulin sensitivity. Regular aerobic exercise, over time, upregulates the sensitivity of GLP-1 receptors throughout the body, meaning the same amount of GLP-1 produces a stronger metabolic effect.
From a chronotherapy standpoint, post-meal movement is particularly potent. It aligns with your body's post-prandial hormonal window, amplifying the GLP-1 signal at exactly the time it is naturally elevated.

One of the simplest and most evidence-supported things you can do for your metabolic health costs nothing and requires no prescription: take a walk after your meals. Post-meal movement — even just 15 to 20 minutes of brisk walking — amplifies your body's natural GLP-1 response, improves blood sugar control, and sends a powerful signal to your metabolic system that everything is working as it should. It is the kind of prescription that fits perfectly in a pocket.
The Bigger Picture
The pharmaceutical advances in GLP-1 receptor agonists — and the newer multi-hormonal agents combining GLP-1 with GIP, glucagon, amylin, and PYY signals — are genuinely remarkable achievements in medicine. For people with significant obesity or type 2 diabetes who need them, these medications can be life-changing and are well-supported by evidence.
But the deeper lesson these medications teach us is this: the hormonal systems your body already possesses are extraordinarily powerful when they are supported rather than undermined. The recipe for activating your own GLP-1 system is not exotic or expensive — it is whole food fiber, quality protein, olive oil, consistent meal timing, post-meal movement, and restorative sleep. These are not alternatives to modern medicine; they are the foundation upon which good metabolic health is built, with or without pharmacological support.
Your gut is producing GLP-1 right now. The question is whether your next meal, your next bedtime, and your next walk after dinner will give it the signal it needs to do its best work.
Dr. Gina Estupinan.
Your body is already equipped with the tools for metabolic health — sometimes it just needs the right timing, the right foods, and a little encouragement to use them.

References
- 1.Drucker DJ. (2006). The biology of incretin hormones. Cell Metabolism, 3(3), 153–165.
- 2.Holst JJ. (2007). The physiology of glucagon-like peptide 1. Physiological Reviews, 87(4), 1409–1439.
- 3.Lim EL, et al. (2011). Reversal of type 2 diabetes: normalisation of beta cell function in association with decreased pancreas and liver triacylglycerol. Diabetologia, 54(10), 2506–2514.
- 4.Chambers ES, et al. (2015). Effects of targeted delivery of propionate to the human colon on appetite regulation, body weight maintenance and adiposity in overweight adults. Gut, 64(11), 1744–1754.
- 5.Fernandez-Twinn DS, et al. (2019). Protein intake and GLP-1 secretion: mechanistic insights. Nutrients, 11(3), 644.
- 6.Sutton EF, et al. (2018). Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metabolism, 27(6), 1212–1221.
- 7.Jakubowicz D, et al. (2013). High caloric intake at breakfast vs. dinner differentially influences weight loss of overweight and obese women. Obesity, 21(12), 2504–2512.
- 8.Vollmers C, et al. (2012). Time of feeding and the intrinsic circadian clock drive rhythms in hepatic gene expression. PNAS, 109(44), 17684–17689.
- 9.Cani PD, et al. (2009). Gut microbiota fermentation of prebiotics increases satietogenic and incretin gut peptide production with consequences for appetite sensation and glucose response after a meal. American Journal of Clinical Nutrition, 90(5), 1236–1243.
- 10.Kerry Health and Nutrition Institute. (2026, January 22). The Next Wave of GLP-1 Treatments.
- 11.Martchenko A, et al. (2020). Circadian rhythms and the gastrointestinal tract: relationship to metabolism and gut hormones. Endocrinology, 161(12), bqaa167.
- 12.Zhao L, et al. (2018). Gut bacteria selectively promoted by dietary fibers alleviate type 2 diabetes. Science, 359(6380), 1151–1156.
