How Breathwork Impacts Your Mental Health and Stress Resilience
The Science Behind Your Breath and Why It May Be a Cost-Effective Tool You're Not Using
Breathwork is far more than a relaxation technique — it's a physiologically profound practice that reshapes your nervous system, modulates inflammation, and builds lasting stress resilience. Here's what the science says, and how to put it into practice.

You do it roughly 22,000 times a day, yet for most of us, it happens entirely on autopilot. Breathing — the most fundamental act of being alive — turns out to be one of the most underutilized levers we have for reshaping our mental health, regulating our stress response, and even modifying our biology at a cellular level. As a physician with a deep interest in functional medicine and lifestyle-based interventions, I find the science of breathwork genuinely intriguing, because it sits at a rare intersection: it is simultaneously ancient, evidence-backed, accessible, and profoundly effective.
In this post, we're going to take a serious look at how different breathwork practices impact your physiology, from your autonomic nervous system all the way down to your cells, and connect that science to practical techniques you can begin using today.
The Autonomic Nervous System: Your Body's Stress Control Panel
Before we dive into specific breathing techniques, it helps to understand the physiological landscape they operate in. Your autonomic nervous system (ANS) governs everything that happens in your body without conscious effort — heart rate, digestion, immune activation, hormonal release. It has two primary branches: the sympathetic nervous system (SNS), often called the "fight-or-flight" system, and the parasympathetic nervous system (PNS), sometimes called the "rest-and-digest" system.
Chronic psychological stress keeps the SNS in a state of persistent low-grade activation. Cortisol and adrenaline flood your system, blood pressure creeps up, digestion slows, sleep quality degrades, and inflammatory markers rise. Over time, this chronic sympathetic dominance has been linked to depression, anxiety disorders, cardiovascular disease, metabolic dysfunction, and immune dysregulation; a cascade of downstream consequences that begins with something as seemingly mundane as a dysregulated stress response.
Here is the extraordinary part: breathing is the only autonomic function you can also control voluntarily. That means your breath is a direct, bidirectional bridge between your conscious mind and your autonomic nervous system. When you deliberately change how you breathe, you are not just changing the air in your lungs — you are actively modulating neurochemistry, heart rate variability (HRV), and the hormonal environment of your entire body.

The vagus nerve is the anatomical superstar of this story. As the longest cranial nerve in the body, it carries parasympathetic signals from your brainstem down through your throat, lungs, heart, and abdominal organs. Roughly 80% of the signals traveling along the vagus nerve are afferent — meaning they travel upward, from the body to the brain. This means your body is constantly sending status reports to your brain, and the quality of those reports depends enormously on the state of your physiology.
Slow, rhythmic, diaphragmatic breathing directly stimulates vagal afferent fibers in the lungs and heart, triggering a cascade of parasympathetic activation that can lower cortisol, reduce heart rate, and shift brain activity toward calmer, more regulated states.
Clinically, the strength of this vagal tone is measurable as heart rate variability (HRV) — the slight variation in time between heartbeats. Higher HRV is consistently associated with better emotional regulation, cognitive flexibility, lower anxiety, and reduced cardiovascular risk. Breathwork, practiced regularly, is one of the most reliable non-pharmacological tools for improving HRV.
Diaphragmatic Breathing: The Foundation of It All
Most adults breathe shallowly into the upper chest, a pattern reinforced by sedentary postures, stress, and even tight clothing. This so-called "thoracic breathing" is associated with higher respiratory rates, reduced oxygen efficiency, and greater sympathetic activation — essentially, it keeps your body in a low-grade alert state.
Diaphragmatic breathing, by contrast, engages the dome-shaped muscle at the base of your lungs to create a deeper, slower breath. When the diaphragm descends on inhalation, it increases intra-abdominal pressure and stimulates the baroreceptors in the aorta and carotid arteries — pressure sensors that signal the brain to reduce sympathetic output and increase parasympathetic tone. The physiological result is measurable within minutes: lower blood pressure, reduced cortisol, slower heart rate, and a subjective sense of calm.
Practically, diaphragmatic breathing is the entry point for almost every structured breathwork protocol. To practice it: place one hand on your chest and one on your abdomen. Inhale slowly through your nose, directing the breath so your abdomen rises while your chest stays relatively still. Exhale fully. Even five minutes of this, practiced daily, can begin to shift your baseline autonomic tone over weeks.
Box Breathing and Resonance Frequency Breathing: Engineering Calm
Once you have diaphragmatic breathing as your foundation, more structured techniques can be layered on top. Two of the best-researched are box breathing and resonance frequency (coherence) breathing.
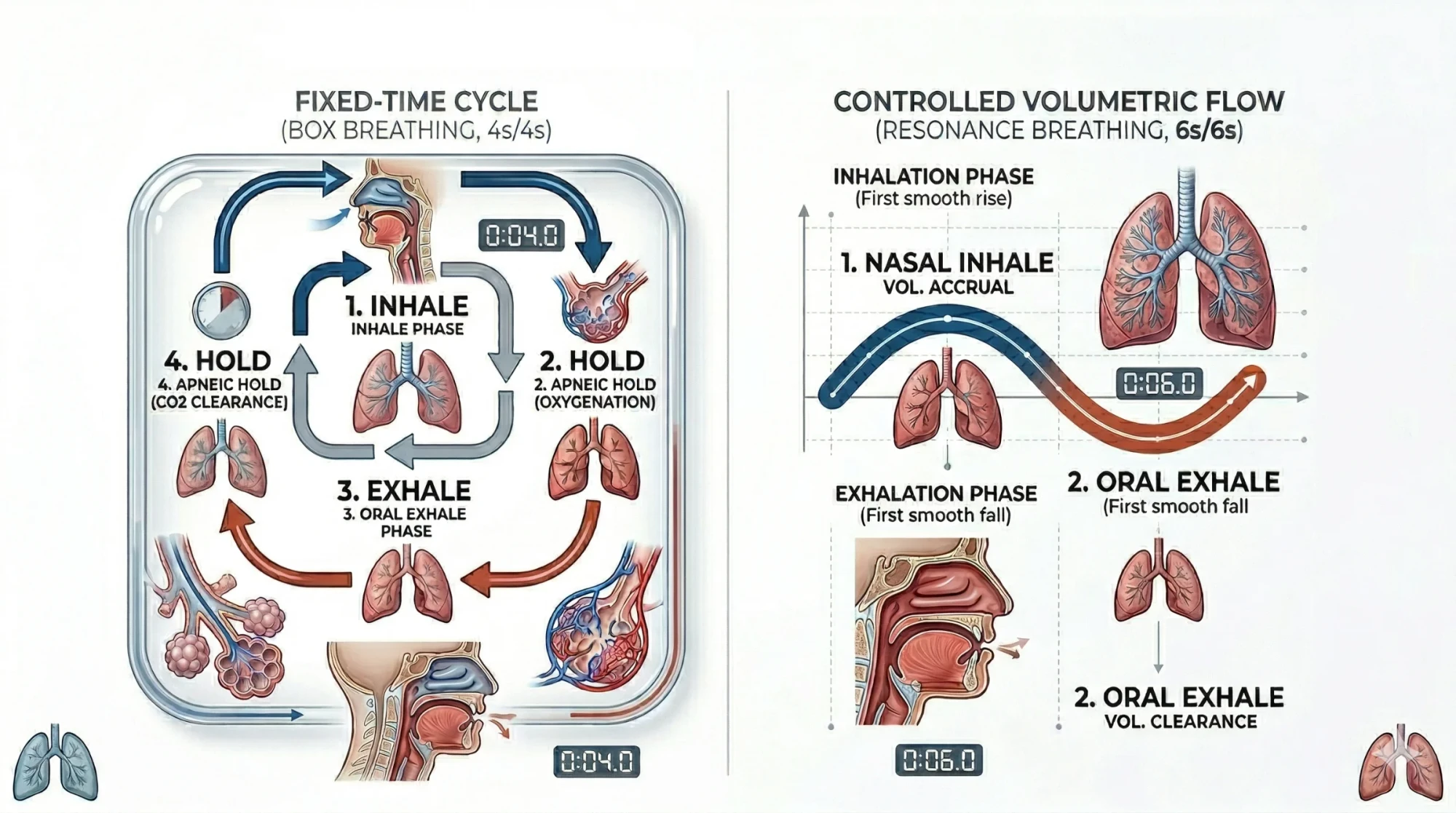
Box breathing — popularized in high-performance contexts including military and surgical settings — involves a four-count inhale, a four-count hold, a four-count exhale, and a four-count hold before the next breath. The symmetrical rhythm and the breath holds activate the Hering-Breuer reflex, a stretch-receptor response in the lungs that amplifies vagal output. Research in high-stress professionals has shown that regular box breathing practice reduces perceived stress scores, lowers cortisol, and improves cognitive performance under pressure. If you find yourself in an acute stress response — elevated heart rate, tunnel vision, racing thoughts — four rounds of box breathing can interrupt the SNS cascade and restore prefrontal cortical function within minutes.
Resonance frequency breathing, sometimes called coherent breathing, involves breathing at a rate of approximately five to six breath cycles per minute (roughly a five-second inhale and a five-second exhale). This specific rate creates a phenomenon called cardiovascular resonance, where the respiratory cycle aligns with the Mayer wave — a natural oscillation in blood pressure — maximizing baroreflex sensitivity and producing the largest possible swing in HRV. Clinical trials have demonstrated meaningful reductions in symptoms of depression and PTSD using resonance frequency biofeedback protocols. Even without biofeedback equipment, approximating this rhythm through a five-count in, five-count out pattern can produce measurable parasympathetic benefit.
Carbon Dioxide, Oxygen, and the Chemistry of Your Cells
Here is where breathwork gets genuinely fascinating from a physiological standpoint — and where it sometimes contradicts intuition. Most people assume that breathing more, faster, or deeper must always be better for oxygenation. In reality, the relationship between breathing and cellular oxygen delivery is governed by a principle called the Bohr Effect.
Your red blood cells carry oxygen bound to hemoglobin. The degree to which they release that oxygen to your tissues depends critically on the partial pressure of carbon dioxide (CO₂) in the blood. When CO₂ is low — as happens with chronic over-breathing or hyperventilation — hemoglobin holds onto oxygen more tightly, and tissues paradoxically receive less oxygen despite adequate blood oxygen saturation. This is the Bohr Effect, first described by Danish physiologist Christian Bohr in 1904, and it has profound implications for both mental and physical performance.
Chronic low-grade hyperventilation is more common than most people realize and is closely associated with anxiety disorders, panic attacks, and chronic fatigue. Individuals who habitually over-breathe develop a lower CO₂ tolerance set point, meaning their nervous system triggers an alarm response — dizziness, tingling, shortness of breath — at CO₂ levels that are objectively normal. Breathwork methods that emphasize nasal breathing, reduced breath volume, and extended exhales are partly corrective through their ability to recalibrate this set point over time.
Nasal breathing deserves specific mention here. The nasal passages produce nitric oxide (NO), a vasodilatory molecule that relaxes smooth muscle in blood vessels and airways, improves oxygen uptake in the lungs by up to 10–15%, and has direct antimicrobial and anti-inflammatory properties. Switching from habitual mouth breathing to nasal breathing — during rest, exercise, and sleep — may be one of the highest-leverage, lowest-cost interventions available for improving cardiovascular health, immune function, and cognitive performance.
The HPA Axis, Cortisol, and Breathwork's Impact on Chronic Stress
Beyond the immediate ANS effects, regular breathwork practice appears to modulate the hypothalamic-pituitary-adrenal (HPA) axis — the neuroendocrine system that controls the cortisol stress response. Prolonged psychosocial stress dysregulates this axis, leading to either chronically elevated cortisol (associated with anxiety, insomnia, weight gain, and immune suppression) or blunted cortisol output (seen in burnout and chronic fatigue).
Studies examining yoga-based and slow breathing interventions have consistently shown reductions in salivary cortisol and improvements in perceived stress over intervention periods of four to eight weeks. The proposed mechanism involves vagal stimulation reducing hypothalamic CRH (corticotropin-releasing hormone) secretion, dampening the initial trigger of the cortisol cascade. Additionally, GABA — a primary inhibitory neurotransmitter whose deficiency is implicated in anxiety and mood disorders — appears to increase following yoga breathing practices, a finding that has drawn attention from researchers interested in non-pharmacological approaches to anxiety management.

One particularly elegant dimension of breathwork is its impact on inflammatory biology. Stress-induced SNS activation promotes the release of pro-inflammatory cytokines — molecular messengers like IL-6 and TNF-alpha — through both direct neural pathways and the cortisol-driven suppression of immune regulation. The vagus nerve, via what researchers call the "inflammatory reflex," exerts a counter-regulatory influence on this process: vagal efferent signals activate splenic macrophages to suppress cytokine release, damping systemic inflammation. Breathwork practices that enhance vagal tone may therefore be contributing to anti-inflammatory effects that extend well beyond the nervous system, with potential implications for conditions ranging from depression (increasingly understood as an inflammatory disorder) to autoimmune disease.
Cyclic Sighing, the Extended Exhale, and Real-Time Stress Relief
Not all breathwork requires a dedicated practice session. One of the most intriguing recent findings in respiratory neuroscience concerns the cyclic sigh — a pattern in which a normal inhale is followed by a second, brief top-up inhale before a long, slow exhale. This double-inhale re-expands atelectatic (partially collapsed) alveoli that build up during normal tidal breathing, and the subsequent extended exhale produces the largest and most rapid shift in autonomic state available through breathing alone.
Research from the Stanford School of Medicine published in 2023 compared cyclic sighing, box breathing, and mindfulness meditation over a four-week period. Cyclic sighing produced the greatest and most rapid reductions in anxiety and negative affect, as well as the most significant improvements in HRV and resting respiratory rate. The protocol is elegantly simple: two inhales through the nose (the second is a short sniff to fully inflate the lungs), followed by a long, slow exhale through the mouth. Practicing this five minutes per day appears to be sufficient to produce measurable mood and physiological benefits.
The extended exhale is a recurring principle across multiple effective techniques, and its mechanism is consistent: exhalation preferentially activates the parasympathetic branch of the ANS through increased vagal tone during the down-phase of the respiratory cycle. This is why simply making your exhales longer than your inhales — even without any formal protocol — produces a rapid calming effect. A 4-7-8 breath (four counts in, seven-count hold, eight-count exhale) leverages this principle aggressively and is among the most effective acute interventions for pre-sleep anxiety or acute stress responses.
Putting It Into Practice: A Tiered Approach
Given the breadth of techniques available, it helps to think about breathwork in tiers based on your goals and the time you have available.
Tier 1 — Daily Foundation (5 minutes): Begin each morning with five minutes of diaphragmatic nasal breathing at a slow, deliberate pace. This alone, practiced consistently, will begin to shift your HRV baseline and cortisol pattern over weeks. It also re-establishes nasal breathing as your default, with the downstream benefits of nitric oxide production and improved CO₂ tolerance.
Tier 2 — Acute Stress Interruption (1–3 minutes): Keep box breathing or cyclic sighing in your toolkit for acute stress moments — before a difficult conversation, during a demanding workday, or when anxiety spikes. These work within minutes and require no equipment or quiet environment.
Tier 3 — Dedicated Practice (15–20 minutes, 3–5 times per week): Resonance frequency breathing or a structured slow-breathing protocol practiced at depth produces the most robust and lasting physiological adaptations, including meaningful HPA axis recalibration, sustained HRV improvement, and anti-inflammatory effects. Apps and biofeedback devices that measure HRV in real time can help you identify your personal resonance frequency and track progress objectively.
Tier 4 — Advanced and Exploratory (with appropriate guidance): Techniques like Wim Hof breathing, holotropic breathwork, or tummo breathing produce intense physiological states and warrant supervised introduction. These are not appropriate starting points for most people, particularly those with cardiovascular conditions, epilepsy, or a history of psychosis.
The Mental Health Dimension: Beyond Stress Reduction
It would be an oversimplification to frame breathwork purely as a stress management tool. The evidence base is expanding into clinically meaningful territory across several mental health domains.
In anxiety disorders, slow breathing interventions reduce trait anxiety scores and attenuate the physiological startle response. The proposed mechanism involves both HPA axis normalization and top-down prefrontal modulation of amygdala reactivity — in other words, a calmer body sends calmer signals to the brain's threat-detection system, and over time, that system becomes less hair-trigger responsive.
In depression, particularly forms with high inflammatory burden or HPA dysregulation, slow breathing and yoga pranayama practices have shown antidepressant effects in randomized controlled trials, with effect sizes comparable to standard antidepressant medications in some studies — though it is important to note that breathwork should be considered an adjunct to, rather than a replacement for, established treatment in moderate-to-severe depression.
In post-traumatic stress, the ability of breath-focused practices to dampen the physiological hyperarousal that characterizes PTSD — the chronically elevated SNS tone, exaggerated startle response, and hypervigilance — is particularly well-suited to the disorder's neurobiology. The combination of somatic downregulation through breath with trauma-focused psychotherapy is an increasingly mainstream approach in trauma treatment.
Finally, emerging evidence suggests that consistent breathwork practice improves sleep quality — both subjectively and objectively, as measured by polysomnography — by reducing pre-sleep cortisol, lowering core body temperature through parasympathetic vasodilation, and supporting the transition into slow-wave sleep stages where cellular repair and memory consolidation occur.
A Physician's Perspective: Why I Recommend This to Almost Every Patient
What strikes me most about breathwork, from a functional medicine standpoint, is the remarkable ratio of benefit to cost. It requires no prescription, no equipment for most protocols, no financial investment, and no significant time commitment to begin experiencing physiological benefit. It is one of the few interventions that simultaneously addresses the nervous system, the endocrine system, the immune system, and the respiratory system — often within a single practice session.
I recommend some form of structured breathing practice to virtually every patient I see dealing with chronic stress, anxiety, poor sleep, or inflammatory conditions. Not as a replacement for medical care, but as a powerful adjunct that works through mechanisms we now understand reasonably well — and that patients consistently report as empowering, because it places an effective tool directly in their own hands.
Your nervous system is not fixed. Your stress response is not an immutable trait. The degree of vagal tone you carry into each day, the HRV signature of your heart, the cortisol rhythm of your HPA axis — all of these are dynamic, plastic, and responsive to practice. Breathwork is one of the clearest demonstrations of this neuroplasticity in action. It is, quite literally, a way of training your biology to be more resilient.
Dr. Gina Estupinan.
Your next breath is an opportunity. Use it intentionally, and let it change your biology — one inhale at a time.

References
- 1.Balban MY, Neri E, Kogon MM, Weed L, Nouriani B, Jo B, Holl G, Zeitzer JM, Spiegel D, Huberman AD. (2023). Brief structured respiration practices enhance mood and reduce physiological arousal. Cell reports. Medicine, 4(1), 100895. https://doi.org/10.1016/j.xcrm.2022.100895
- 2.Dillard, C. C., Martaindale, H., Hunter, S. D., & McAllister, M. J. (2023). Slow Breathing Reduces Biomarkers of Stress in Response to a Virtual Reality Active Shooter Training Drill. Healthcare, 11(16), 2351. https://doi.org/10.3390/healthcare11162351
- 3.Mirgain, S. A., Singles, J., & Hampton, A. (2016, May 1). The power of breath: Diaphragmatic breathing. U.S. Department of Veterans Affairs. https://www.va.gov/WHOLEHEALTHLIBRARY/tools/diaphragmatic-breathing.asp
